AskAwayHealth
Beyond Pink Ribbons – Taking Action Against Breast Cancer
April 26, 2023

What can you do to reduce your breast cancer risks? Let’s take a look at the risks that can’t change but, more importantly – those you can do something about!
What is breast cancer? Simply put, it’s when abnormal cells form in the breast and begin to grow and divide in an uncontrolled way.
They will continue to grow and spread to other tissues causing damaging symptoms.
Why look at women’s breast cancer risks after 40 years?
Breast cancer can happen under 40 but is more common as we age.
Around this midlife stage, many risk factors – those things that increase our risk for disease – are established.
Many women are approaching menopause, and some of us may experience difficult symptoms and need to change our lifestyles.
So this is an excellent time to think again about your risks if you still need to do so.
- Know your family history
- Maintain a healthy weight
- Stay physically active
- Limit alcohol intake
- Don’t smoke
- Breastfeeding
- Get regular mammograms
- Consider other screening tests
- Reduce radiation exposure
- Limit hormone therapy
- Eat a healthy diet
- Manage stress
- Chemicals and environmental factors
- Breast types
- Early breast changes
- Timing of periods starting/stopping
- Sex hormones
- Ethnicity
- Previous cancer
- Height
- Having children or not
Here are factors that can determine if you develop breast cancer. In addition, we share some steps that may help to reduce your breast cancer risk:
Know your family history
Women with a family history of breast cancer are at higher risk, so it’s essential to be aware of your family’sfamily’s medical history.
Having a family history of breast cancer means you have a higher risk of developing breast cancer than the general population because other family members have had breast cancer.
Having a mother, sister or daughter diagnosed with breast cancer increases the risk of breast cancer.
This risk is higher when more close relatives have breast cancer or if a relative developed breast cancer under 50.
But most women with a close relative with breast cancer will never develop it.
A related problem is some people have an increased risk of breast cancer because they have an inherited faulty gene.
Several gene faults can increase breast cancer risk, and there are tests for some of them.
A faulty gene means you are more likely to get breast cancer than someone who doesn’t. But it is not a certainty.
Two of these faulty genes are known as BRCA1 and BRCA2.
These are rare.
According to Cancer Research UK, only about 2 out of every hundred (about 2%) breast cancers are related to a change in the BRCA1 or BRCA2 genes.
Maintain a healthy weight
Obesity and being overweight are risk factors for breast cancer, especially after menopause.
So lower your BMI to the NHS-recommended healthy BMI range of 18.5 to 24.9.
In addition, consider what you eat and drink and how active you are. Let’s be clear that being fat does have health implications.
We should not politicise or play being woke about the harmful effects of excess weight.
Stay physically active
Regular exercise can help to lower your breast cancer risk. Aim for at least 30 minutes of moderate physical activity most days of the week.
Being physically active helps reduce your risk of breast cancer and has other health benefits.
For example, exercise enables you to lose weight. In addition, it is associated with reduced inflammatory activities, which lead to abnormal cells developing and growing.
Doing at least 150 minutes of moderate physical activity, such as brisk walking or gardening, or at least 75 minutes of vigorous physical exercise, such as running or cycling, each week is recommended.

Limit alcohol intake
Drinking alcohol increases your breast cancer risk, so it’s recommended that women limit their alcohol intake to no more than one drink per day.
This risk increases with each extra unit of alcohol per day. The number of units in a drink depends on the size of the drink and the volume of the alcohol.
Better to drink alcohol rarely or in moderate amounts on social occasions. If you must drink more often than that, then not more than 14 units/week.
Don’t smoke
Smoking is a known risk factor for many types of Cancer, including breast cancer.
Studies suggest that smoking, especially if started at a younger age, can moderately increase breast cancer risk and harm overall health.
Breastfeeding
Women who breastfeed for one year or more over their lifetime have a lower risk of breast cancer.
Having children under 30 lowers your risk of breast cancer.
Breastfeeding your children for at least six months further reduces breast cancer risk; the longer you breastfeed, the better. This benefit still applies if you start having children later in life.
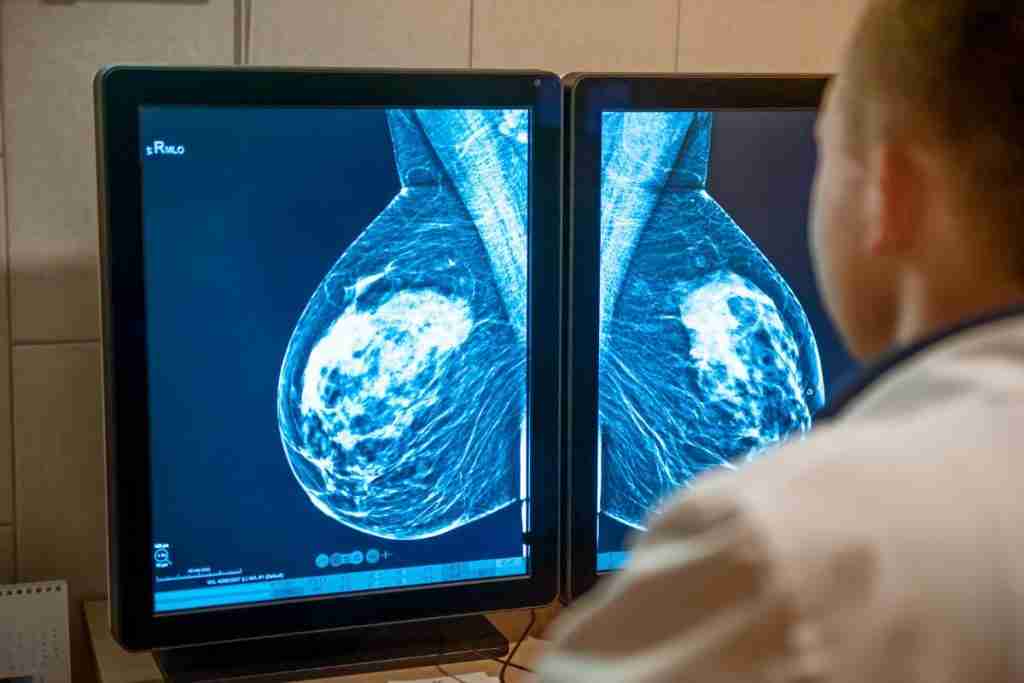
Get regular mammograms
Mammograms can help to detect breast cancer early when it’sit’s most treatable.
A mammogram is an imaging test that uses low-dose X-rays to create images of breast tissue.
The breast is compressed between two plates during a mammogram, and an X-ray is taken. The compression helps to spread out the breast tissue, making it easier to see any abnormalities in the breast.
Mammograms can help detect breast cancer early when it is more treatable.
However, mammograms can miss some cancers, particularly in women with dense breast tissue.
Therefore, additional screening tests, such as breast ultrasound or breast MRI, may be recommended for women with dense breast tissue or other risk factors for breast cancer.
The frequency of mammography screening depends on an individual’sindividual’s age and risk factors for breast cancer.
The American Cancer Society recommends that women with an average risk of breast cancer begin having yearly mammograms at age 45 and continue to have annual mammograms until age 54.
After age 55, women may continue with yearly mammograms or switch to every two years.
In the UK, the National Health Service (NHS) Breast Screening Programme recommends that women between the ages of 50 and 70 should have a mammogram every three years.
This age range is chosen because the risk of developing breast cancer increases with age, and most breast cancers are diagnosed in women over 50.
Women over the age of 70 are still eligible for mammography screening, but they will not automatically receive invitations. However, they can self-refer for screening by contacting their local breast screening unit.
Women with a higher risk of breast cancer, such as those with a family history of the disease or those with certain genetic mutations, may need to start screening earlier and/or have more frequent mammograms or additional screening tests.
Consider other screening tests
Women at high risk of breast cancer may benefit from additional screening tests, such as breast MRI.
Examples are:
Clinical breast exam: This is usually where it starts. A clinical breast exam is a physical examination of the breast tissue by a healthcare provider. It may be recommended in addition to mammography for women with a high risk of breast cancer.
Breast MRI: Magnetic resonance imaging (MRI) is a type of imaging test that uses a magnetic field and radio waves to create detailed images of the breast tissue.
It is more sensitive than mammography and may be recommended for women with a high risk of breast cancer, such as those with a strong family history of the disease or those with specific genetic mutations.
Breast ultrasound: Ultrasound uses sound waves to create images of the breast tissue. It may be recommended in addition to mammography for women with dense breast tissue, which can make it more challenging to detect breast cancer on a mammogram.
Genetic testing: Genetic testing may be recommended for women with a strong family history of breast cancer or those with other risk factors. Genetic testing can help identify specific genetic mutations that increase the risk of breast cancer.
What about examining your breasts?
Some scientists suggest: Breast self-exams (BSE) are no longer routinely recommended for breast cancer screening.
This is because studies have not found evidence that BSEs reduce the risk of dying from breast cancer. Additionally, BSEs can lead to unnecessary biopsies and other procedures for lumps that are benign.
However, women should still be aware of how their breasts usually look and feel and report any changes to their healthcare provider. Regular clinical breast exams (CBEs) by a healthcare provider are recommended for women in their 20s and 30s.
In some countries, mammograms are recommended for women starting at age 40 (or earlier if they have a high risk of breast cancer).
Reduce radiation exposure
High doses of radiation can increase breast cancer risk, so it’s important to limit exposure when possible.
Sources medical imaging – X-rays including mammograms or CT scans – but the radiation exposure with these tests is very low.
There can also be exposure to medical treatments like radiotherapy for conditions like breast cancer.
Having treatment for one breast can increase the risk of cancer in the other breast by a small amount. You will need to weigh this risk against the risk of treating the original cancer.
Home – living near mining operations and contaminated sites.
Workplace – nuclear power, radiology, some types of manufacturing.
Remember, the risk of developing breast cancer from radiation exposure is generally low for most people.
But if you have a family history of breast cancer or other risk factors, discuss your concerns with a healthcare provider.
Limit hormone therapy
Hormone therapy used to manage menopause symptoms can increase breast cancer risk, so women should talk to their doctors about the benefits and risks of hormone therapy.
We have 2 main types of HRT: Oestrogen only or combined HRT with Oestrogen and Progesterone.
The risk of breast cancer increases for women after menopause using any HRT. But it is greatest for those using combined HRT.
The cancer risk is also higher in those using HRT for over 5 years. And for these women, the risk remains increased for at least 10 years after they stop using it.
HRT can have some health benefits apart from easing some menopause symptoms.
They include bone protection, reduced risk of dementia, and some heart disease. It can also help to improve sleep, sex drive, and overall health.
What about the pill? Many women who take the pill are in their late teens, twenties and early thirties. But remember that breast cancer is rare in young women.
So a slight increase in this risk when women take the pill means very few extra cases of breast cancer.
Over time, contraceptives containing oestrogen and progesterone slightly increase breast cancer risk while in current use. But the increased risk will go within 2-10 years of stopping use.
Eat a healthy diet
The impact of diet can be tricky to analyse because we eat a combination of different foods.
A diet high in fruits, vegetables, whole grains, and lean protein sources may help reduce breast cancer risk.
Add more fruit and veg into your life. A mix of red, yellow and orange fruit and non-starchy veg are especially good as they are high in carotenoids. Green leafy vegetables, such as spinach and broccoli, are also good options.
Avoid processed meat like sausages/bacon; cut down on red meat.
The International Agency for Research on Cancer classifies red meat as a probable carcinogen.
In addition, some studies have found that eating a lot of red meat increases your risk of breast cancer, especially premenopausal breast cancer.
To reduce your breast cancer risk, eat less red meat as part of a healthier balanced diet.
What about any special diets like keto? Do they provide special protection from breast cancer?
Not really – diet has 2 roles: it gets you to a healthy weight. It adds supplements or nutrients that may help reduce tissue damage from inflammation.

Manage stress
Chronic stress can weaken the immune system and increase inflammation, contributing to cancer risk. Finding healthy ways to manage stress, such as through exercise, meditation, or therapy, may help to reduce breast cancer risk.
Stress – effect on the immune system and inflammation.
- Self-care days
- Take yourself out of toxic, stressful situations or relationships or jobs
- Holidays
- Share responsibility
- Plan ahead
- Family, friends, socialise etc
Chemicals and environmental factors
Cosmetics and Cleaning Products. It is important to know what goes into and onto your body.
Many everyday products contain endocrine-disrupting chemicals (EDCs), such as Parabens, Phthalates, Triclosan and Bisphenols, which affect your hormones and may increase breast cancer risk.
When buying new or replacement cosmetics, check for parabens, phthalates or triclosan ingredients. Similarly, cleaning products used around the house or at work may contain these chemicals.
Increased light at night (from night shifts)may slightly increase your risk of breast cancer, as it lowers your levels of melatonin, a hormone associated with your body clock, which increases breast cancer risk.
Reduce the time you are exposed to light at night and always get good quality sleep.
Organic solvents: There is evidence that long-term exposure to organic solvents, including degreasing agents such as benzene or ethylene glycol used in anti-freeze, increases your risk of breast cancer.
Where you live: Living in an urban environment, such as a city or large town, increases your risk of breast cancer compared to a more rural environment. One reason may be that you are exposed to more air pollution.
When outdoors, try to avoid pollution hotspots such as main roads at rush hours and check pollution levels on weather apps or websites
Sunlight and Vitamin D – Sunlight is the best way to take vitamin D, which is good for overall health. On the other hand, having a vitamin D deficiency may raise your risk of breast cancer.
It is also good to be outside and active, even in the colder months, but always do not spend too long in the sun to protect yourself from skin cancer.
Risks you cannot do anything about
We’ve been looking at risk factors you may be able to address that will make it less likely to develop cancer. But let’s look at others which we cannot change.
These include age and family history – the best defence is being aware of these risks so you can address the ones you can change.
But other risk factors exist and include:
Breast types
Breasts come in all shapes and sizes. Does the type of breast make women more at risk of Cancer?
Breasts are made of different types of tissues, glandular tissue that produces milk, fat tissue and ducts. A woman’s breast becomes less dense the older we get.
However, by their genetic makeup, some ladies have more dense breasts (with less fat tissue) than others.
Those with denser breasts are more at risk of Cancer.
Early breast changes
Women with a diagnosis of DCIS or LCIS have double the usual risk of invasive breast cancer in the same or other breast.
But it is important to remember that most women with LCIS or DCIS will not develop invasive Cancer.
Timing of periods starting/stopping
Early period starting and Late period stopping increase the risk of breast cancer as both expose women to oestrogen for a longer time.
Sex hormones
Your levels of sex hormones (Oestrogen, Progesterone and Testosterone) increase the risk of breast cancer.
Women usually have small amounts of testosterone in their bodies.
However, after menopause, women with higher levels of oestrogen and testosterone than usual in their blood may have a higher risk of breast cancer.
Also, women with higher testosterone levels in their blood before menopause have a higher risk of breast cancer.
Ethnicity
From a large study comes the suggestion that white women are at a higher risk of breast cancer than other ethnic groups- the reason for this has been attributed to lifestyle factors.
Previous cancer
Having previous Cancer in one breast puts you at greater risk of Cancer in the same breast or the other. This means strict monitoring is required.
Having other cancers like skin cancer (melanoma), lung, a type of chronic leukaemia, and womb or bowel Cancer also puts you at higher risk of breast cancer.
Height
Although the reason is unclear, women taller than average have a slightly increased risk of breast cancer after menopause. It may be thanks to different hormone levels in taller women.
Having children or not
For many women, this is out of their control.
Women with children have a slightly lower risk of breast cancer than women who don’t. The risk reduces further the more children you have.
Your age when you have your first child also has an effect. The younger you are when you have your first child, the lower your risk.
More Reading
Editing by AskAwayHealth Team
Disclaimer
All AskAwayHealth articles are written by practising Medical Practitioners on various healthcare conditions to help promote quality healthcare. The advice in our material is not meant to replace a qualified healthcare practitioner’s management of your specific condition.
To discuss your condition, please get in touch with a health practitioner or reach us directly
Image Credits: Canva
Want to know how your comment data is processed? Learn more

Leave a comment
Please fill in the field below to add a comment.