AskAwayHealth
Don’t Risk It: How To Spot an Ectopic Pregnancy and Prevent Future Complications
July 8, 2020
An ectopic pregnancy is one where the growing baby develops outside the womb. This is a big problem. How do you know if you are having one, and can you prevent it?
Introduction (What’s an Ectopic Pregnancy)
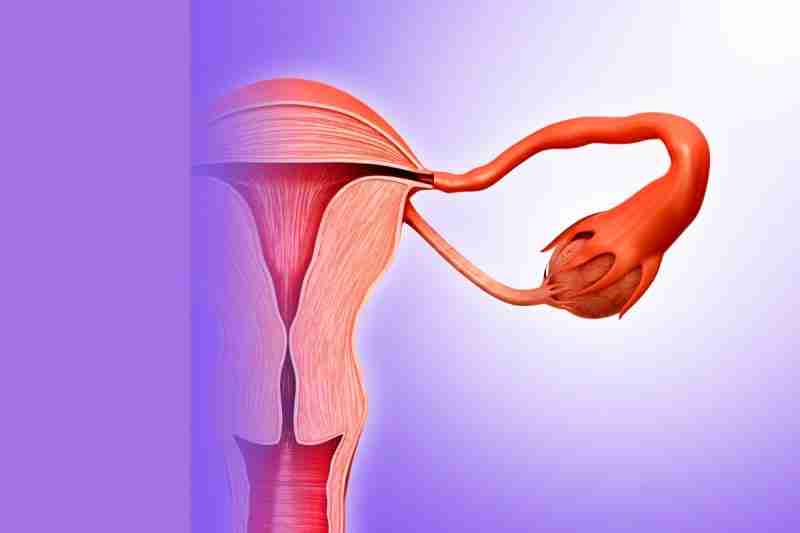
Ectopic pregnancy means ‘misplaced pregnancy’ and most often happens in the fallopian tube, which connects the ovary to the womb.
Following sex, the egg fertilised by sperm begins to develop into the embryo.
The embryo swims up from the vagina into the womb, where it will typically ‘take root’ or implant within its lining till birth.
The mass of tissues from the fertilised egg continues to divide and grow – from an embryo taking the form of a human foetus.
This is the best place for it to grow over the next 9 months.
But sometimes, this doesn’t happen, and the foetus ends up outside the womb, where it cannot survive.
An ectopic pregnancy could also develop in other areas: the ovary, the neck of the womb or even freely within the abdomen.
These are much less common than tubal pregnancy.
Who is Most Likely to Have an Ectopic Pregnancy
Any of the following conditions may increase the risk of an Ectopic Pregnancy:
- A woman who has had a PID (Pelvic Inflammatory Disease) – a womb infection that develops most often following a sexually transmitted infection.
- Older age at pregnancy – from age 35-40 years
- Smoking.
- If you have had an ectopic pregnancy before, you are more likely to have one again.
- The risk increases if you have had two previous ectopic pregnancies.
- Women undergoing IVF – This happens from taking drugs that stimulate the release of eggs from the ovary.
- Having had surgery to the fallopian tube before – such as sterilisation.
- Falling pregnant while using a ‘coil’ – Copper coil (Intrauterine Device) or IUS (Intrauterine System like Mirena or Skylar).
- These are very effective at preventing pregnancy – but on the RARE occasion a woman falls pregnant with them, she may be at an increased risk of having an ectopic pregnancy.
- If you have a condition like endometriosis that causes inflammation of the womb or surrounding areas
- The inflammation increases the risk of scars forming, making it likely for an ectopic pregnancy.
Well, we can’t yet prevent ectopic pregnancy from happening, but we can reduce certain things that could cause it.
- For instance, using a condom when having sex to prevent sexually transmitted infections that cause PID.
- Having Chlamydia and Gonorrhoea infections increase the risk of having an ectopic.
- Another preventive measure is stopping smoking.
When do Ectopic Pregnancy Symptoms start?
For a woman with a regular period who has conceived, 6 weeks of pregnancy is around 2 weeks after the missed period.
Symptoms could happen most often around 6 weeks of pregnancy (if there are symptoms).
However, they may happen anything from 4 – 12 weeks.
Ectopic Pregnancy symptoms include:
- Sudden sharp low abdominal pain to one side – but it may also start as mild pain and build in severity over a few days
- Feeling dizzy, faint or lightheaded.
- Bleeding from the vagina or a brown discharge.
- Bleeding may be heavier or lighter than a usual period, or in some cases, may appear to be a ‘late period’.
- Check out other causes of early pregnancy bleeding here
- Pain when going to the toilet for a poo or to wee.
- Pain to your shoulder tip suggests internal bleeding leaking into the abdomen and irritating the diaphragm at the top.
Diagnosis of Ectopic Pregnancy
Mostly there are no symptoms, and are first seen after a routine ultrasound scan.
If you have symptoms that suggest an Ectopic Pregnancy, you must seek urgent medical attention.
A urine test confirms pregnancy, but a blood test can do more.
With a blood test, in addition to levels of Beta HCG (Human Chorionic Gonadotrophin) showing pregnancy, we can monitor the levels to confirm the status of the pregnancy.
In a healthy pregnancy, BHCG levels continue to go up progressively in the first trimester.
In an ectopic pregnancy, this does not happen, the levels do not go up as quickly, or they fall.
Outcomes from Ectopic Pregnancy
An ectopic pregnancy does not ever survive. There are three possible outcomes.
Scenario 1
First, it may die after settling into the tube for a few days.
Since it does not have the specialised cells like the uterus to care for a viable pregnancy, the foetus cannot survive.
Most often, when the pregnancy dies in the tube, it hardly causes any symptoms.
This may be some light vaginal bleeding or pain, which could be similar to a miscarriage or a late period.
No further action is taken unless symptoms suggest otherwise.
Scenario 2
If the foetus does not die, the pregnancy may continue to grow in the tube, stretching it.
It may be at this point the woman starts to show symptoms – such as pain low in the abdomen towards the affected side, i.e. the tube carrying the foetus.
These symptoms may prompt an ultrasound scan leading to diagnosis and treatment.
Scenario 3 – When Ectopic Pregnancy Ruptures
Finally, a pregnancy continuing to develop within your fallopian tube will split open (rupture) the organ.
This happens because your tube is slim/narrow and only able to stretch a little.
Once this happens, internal bleeding from the burst tube occurs – with severe pain.
The woman may collapse if there is a massive amount of internal bleeding.
This is a medical emergency and needs urgent treatment.
The foetus does not survive, and the mother requires help to stop the bleeding.

After the Diagnosis
Not all ectopic pregnancies result in collapse or emergency admission.
In the case of ruptured ectopic pregnancy, the treatment is emergency surgery to save a life.
The principal aim is to stop internal bleeding.
It is necessary for the removal of the pregnancy and fallopian tube.
In the second case, where the tube has not yet burst the fallopian tube, following diagnosis from the ultrasound scan, treatment is with drugs or surgery.
Surgical Treatment Ectopic Pregnancy
Surgery nowadays is carried out using the keyhole technique, also known as laparoscopy.
Different options are considered:
- Removal of the whole tube or
- Removal of part of the tube.
If your other fallopian tube is already damaged, the surgery will remove the pregnancy and only a portion of the tube – salpingotomy.
When you have a healthy tube, then the entire tube carrying the foetus will be removed – salpingectomy.
Treatment with Drugs
An ectopic pregnancy that has not ruptured the fallopian tube can be treated using drugs.
In this case, the drug, given by injection at a very early stage of pregnancy, kills the pregnancy to stop it from growing in the tube.
While this can work and avoids the option of pregnancy, it does mean a lengthy period of treatment.
This is because even after the injection, you will require regular monitoring to check that the pregnancy is no longer growing and that the fallopian tube is no longer at risk of rupture (bursting).
To achieve this, you will have blood tests every two or three days to check your BHCG levels.
Levels that are falling indicate a pregnancy that is not growing.
You will also have frequent (usually once weekly) ultrasound scans to check on the progress of treatment.
In the last case, where the ectopic pregnancy does not show any symptoms, no further action is needed.
The pregnancy dies before it stretches or damages the tube, and the body takes care of this naturally.
If you have drug treatment for ectopic pregnancy, it is important to be aware that the drug could have side effects such as nausea, vomiting or abdominal pain.
Risks of Pregnancy after Ectopic Pregnancy
Having an ectopic pregnancy and losing a baby is traumatic for a woman and a couple.
Speak to your doctor about counselling support if you think you are struggling.
Following a full recovery from the ectopic pregnancy (whether treatment by drugs/surgery), is it possible to have a healthy pregnancy?
This is possible if you had no health problems or diseases involving your fallopian tube before the ectopic pregnancy.
Having an ectopic pregnancy under these circumstances will not affect your fertility.
However, if you did have problems with conceiving or with the fallopian tube before the ectopic happened, you may be at risk of future problems getting pregnant.
When a woman has surgery to treat an ectopic, she is usually more likely to have fertility problems afterwards than if drugs had been used.
She may even have more ectopic pregnancies in future.
What are My pregnancy chances after my tube is removed?
If the remaining tube is healthy, you have about a 60% chance of future normal pregnancy.
However, you should know that any pregnancy may become ectopic in 10-20% of cases.
So what does this mean?
If you had an ectopic pregnancy, speak to your doctor as soon as you get pregnant again for early monitoring and care.
If you’d like to ask more about ectopic pregnancy, click here.
So an ectopic pregnancy can be life-threatening, but with close attention to your body and early monitoring, this does not need to be the case.
Speak to a doctor or midwife immediately if you develop any ectopic pregnancy symptoms described above.
More Reading
Reference
NICE: Ectopic Pregnancy and Miscarriage
Ectopic Pregnancy: History, Incidence, Epidemiology, and Risk Factors
Mayo Clinic: Ectopic Pregnancy: Signs, Treatment and Future Fertility
Editing by AskAwayHealth Team
Disclaimer
All AskAwayHealth articles are written by practising Medical Practitioners on a wide range of healthcare conditions to provide evidence-based guidance and to help promote quality healthcare.
The advice in our material is not meant to replace the management of your specific condition by a qualified healthcare practitioner.
To discuss your condition, please contact a health practitioner or reach us directly here
